A recent article ‘The Management of Menopause in Women with Philadelphia-Negative Myeloproliferative Neoplasms (MPNs)’ reviews what is currently known about how menopause affects women living with an MPN, and how menopause symptoms can be safely managed in MPN patients. The authors highlight the lack of research and published evidence in this area, and aim to provide practical guidance for clinicians.
The article notes that many women with MPNs are diagnosed in mid-life, when menopausal symptoms commonly begin. Symptoms of menopause and symptoms of MPNs often overlap.
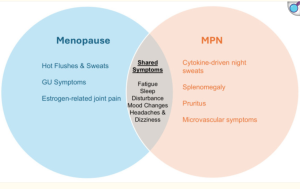
Figure 1: overlapping MPN and menopause symptoms
Key findings from the article are outlined below.
- Symptom overlap is a major clinical challenge, eg hot flushes, night sweats, fatigue, mood changes and cognitive difficulties occur in both menopause and MPNs. This overlap can lead to under-recognition of menopause, misattribution of symptoms to the MPN and reduced quality of life. The authors propose that clinicians should actively consider menopause as a contributor to symptom burden in women with MPNs.
- Thrombosis risk is central to treatment decisions due to the baseline increased risk of blood clots in MPNs. Oral oestrogen increases clotting risk in the general population, transdermal oestrogen (patches, gels) appears to have minimal or no additional clotting risk, progesterone type also matters, with micronised progesterone considered safer.
- Hormone Replacement Therapy (HRT) is not contraindicated, but must be chosen carefully. Cautious, individualised assessment is recommended before prescribing HRT, with transdermal oestrogen likely the safest option. Oral HRT should generally be avoided due to clot risk.
Women with a history of thrombosis or very high-risk disease require extra caution. Decisions should be made collaboratively with haematologists and menopause specialists. - Non-hormonal therapies are important alternatives. Eg, certain antidepressants, gabapentin, cognitive behavioural therapy and lifestyle interventions, especially for women who cannot safely use HRT.
The article proposes a step-by-step clinical pathway for managing menopause in women with MPNs: symptom assessment; evaluation of clotting risk; consideration of HRT vs non-hormonal options; and ongoing monitoring.
For women living with an MPN, the key message is that menopause can be managed safely, and treatment options, including HRT, may still be available with the right clinical oversight.